Managing and Treating Vernal Keratoconjunctivitis – a guide for parents
Posted on 25 February 2022

If your child’s been diagnosed with vernal keratoconjunctivitis – also known as VKC for short – then you probably have lots of questions.
That’s because VKC is rare – it only affects 3.2 people per 10,000 in Western Europe1 – so there’s much less information out there compared to other allergic conditions like eczema or asthma and you’re unlikely to bump into another parent who has a child with it.
You’re not alone if you find that challenging, so to help, we’ve rounded up some of the best tips from other parents and medical specialists across the globe!
We also understand that it can be reassuring to hear from other parents of children with VKC, that’s why we have created our Parents Guide. You can find the booklet, here.
Treatment of Vernal Keratoconjunctivitis
The number one things you can do to help manage VKC is to stay on top of your child’s vernal keratoconjunctivitis treatment – which is usually a type of eye drop.
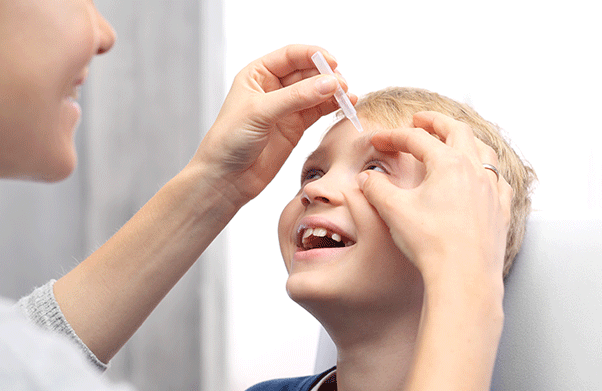
Putting in eye drops
A squirming child and hectic schedule can make this daily chore daunting but don’t worry, it gets easier with practice. Here’s a few tips to get you popping those drops in like a pro2:
- Set-up for success – Take a minute to prep, get a tissue or clean cloth ready and wash your hands
- Tilt-back – Get them to raise their chin but if they’re a bit wobbly or distracted by this, then simply get them to lay down. Or you could get a helper to hold them still!
- Make a pocket – Gently pull down on the bottom eyelid, it makes a little opening for the eye drops
- Mop up – Use the tissue to hold over the eye and clean up any excess but be careful not to wipe the eye drop out of the eye
- Avoid contamination – don’t clean or touch the nib of the eyedropper, just put the lid back on
- Listen – A bit of stinging is normal and doesn’t last long, but if it seems like it’s stinging a lot and your child is very uncomfortable, then talk to your ophthalmologist. They may suggest a different type of drop
- Give it 5 to 10 – If you’ve got another type of drop to give them, try to wait 5 to 10 minutes, but if it’s not possible don’t worry too much as the main thing is to give them their medication
Tip: Keep VKC treatment in multiple locations, like a bag, car glove compartment and around the house so you’ll always have them to hand!
Making medicine time fun
Tears and tantrums don’t have to be a feature of medicine time. Try these parent-tested tips to turn frowns upside down:
- Get them involved – Give them a special job to do for medicine time – maybe that’s as simple as starting a timer so that everyone’s done on time
- Give encouragement – Praise things that went well rather than criticise what wasn’t so good
- Stay positive – Try to smile (even if you don’t feel it) as they’ll pick up on your emotions
- Reward (occasionally) – This can help incentivise a positive attitude, especially when you’re just starting out
- Explain – Why the drops are important (but don’t scare them!). Find out more about the importance of keeping on top of treatments in our blog post, here.
- Use stories – If it helps (perhaps the eye drops give them superpowers?!). Check out our Understanding VKC comic for some inspiration!
- Turn it into a game – When they’re having their drops, give them a task like listing as many different sounds they hear or reciting as many capital cities as they can remember
- Choose a calm environment – Somewhere without lots of distractions where you both feel comfortable. You could even play their favourite song to help them relax
- Don’t dwell on it – If it doesn’t go to plan, relax and know that every parent with a child with VKC has been in a similar position. Smile and let your child know that you’ll nail it next time!

Getting help – when to see the ophthalmologist
In your appointment, you’ll want to agree with your ophthalmologist when they should see your child again, for example, if they get a flare-up or for a routine follow-up. If something is a real struggle or doesn’t feel right, then be sure to contact them.
Tip: Too many sleepless nights are a sign that things are not OK and to check in with your ophthalmologist.2
You can find out more about what happens during an appointment with an ophthalmologist in our blog post, here.
Talking to your child about their VKC
Older children
Some older children can apply their own eye drops. If this is your child, then try to make them aware of how important it is that they take them exactly as directed by the doctor, even if their eyes feel better. This is because eye drops can help prevent symptoms flaring up and causing damage to the eyes.
Tip: Sometimes children will avoid taking medicine at school because they don’t want to feel different. Be sure to explain to them that VKC isn’t contagious and millions of people around the world have used eye drops including some best loved celebrities – Try to find an example of someone they admire!
No matter if your child is independent with their medication or not, the main thing is to talk, talk, talk – Communication is key so that you know how they’re feeling and if the going gets tough, you can get help!
Managing VKC as a family – life hacks and more!
There’s no need for your child to stop doing the things they enjoy. There are things you can do to help avoid flare-ups, but these are small compromises that shouldn’t get in the way of family fun!2,3

- Sunny days – This can be a common trigger for VKC, but getting your child to wear sunglasses and a hat can help
- Holidays – Be aware that the sun, sand and sea can be irritating, so make sure you’ve got a good supply of medication with you just-in-case
- Baking – Cooking up some family cupcakes is heaps of fun, and for children with VKC wearing science goggles can help stop irritating flour from getting in their eyes
- Swimming – There’s no need to avoid this healthy activity, just be sure to pack goggles in their swim kit. If they’re having a flare-up, then take a break from this for a while
- Sleepovers – Explain the condition to friends and parents, including that it isn’t contagious, and that it’s well managed with treatment
- Cold cloths – These can help provide instant relief from itchy symptoms, so keep a few prepped in the fridge as an alternative to them rubbing their eyes
- Bedtime – If this is a time when your child’s eyes are uncomfortable, then try using wet tissues or a silk eye mask to soothe them while they settle down
- Itching urges – Rubbing can make it worse, but having some alternatives on hand can provide relief or at least a distraction – try artificial tears (you can use them as often as needed) or gently pressing a palm over the eye
- School – Some schools will be happy to put eye drops in, others might have policies that mean they can’t administer medicines. Help the teachers and your child to understand the condition so that they’re able to tell others about it
Tip: Create a VKC survival kit to go wherever your child goes:
- A hat
- Goggles
- Sunglasses
- Their medication
- Artificial tear eye drops
- Cooling eye mask
Our Parents Guide contains lots more helpful tried and tested tips and tricks. You can read the booklet, here.
Similar diagnosis – is it a VKC flare-up or something else?
Over time, you’ll get to know the signs of a flare-up and how your child reacts to them:2
- Droopy eye
- Discharge from the eye
- Sticky or watery eyes
- Soreness/itchiness when blinking
- Prolonged or unusual blinking
- Pressing on the eyes
- Difficulty opening eyes, especially in the morning
- Difficulty going out in the light
- Blurred vision
Important note:
Sometimes the symptoms of VKC can be confused with Conjunctivitis (also known as red eye or pink eye) – an infection of the eye and eyelids from bacteria or viruses. Conjunctivitis is contagious and typical symptoms are redness, irritation, a sandy or burning feeling in the eyes, and puss which can cause the eyelids to stick together.3 Doctors can tell if it’s VKC rather than other types of allergic conjunctivitis because VKC doesn’t affect the eyelid margin – that’s the bit on the edge, where the eyelashes grow.4
You can find out more about VKC and VKC symptoms in our blog post, here.



